In Press: Dr. Eithan Kotkowski Publishes First Author Paper on Creutzfeldt-Jakob Disease

 During his rotation through the neurology intensive care unit last year during his third year of medical school, Eithan Kotkowski, Ph.D. and his fellow medical school classmates helped oversee the care of a patient with a case of rapidly-progressive sporadic Creutzfeldt-Jakob Disease (CJD).
During his rotation through the neurology intensive care unit last year during his third year of medical school, Eithan Kotkowski, Ph.D. and his fellow medical school classmates helped oversee the care of a patient with a case of rapidly-progressive sporadic Creutzfeldt-Jakob Disease (CJD).
“CJD is an incredibly rare and devastating disease to both patients and their families,” Dr. Kotkowski explained. “It is a progressive neurodegenerative disease with no known cure caused by the buildup of prions, abnormally folded infectious proteins similar to those that cause Mad Cow Disease.”
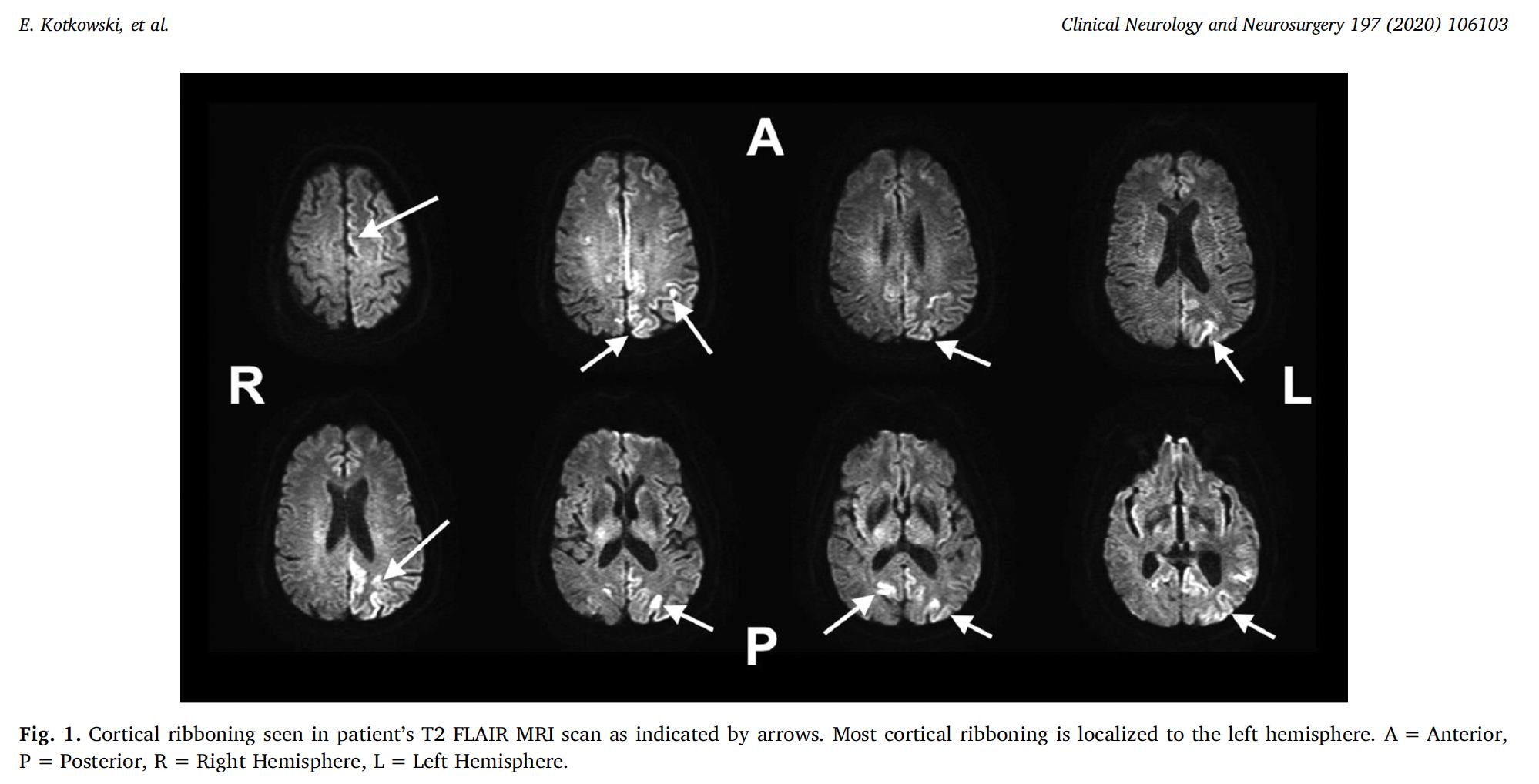
This buildup of prions leads to rapid changes in the brain manifesting as “cortical ribboning” on MRI (shown below), changes in cognition and behavior, and death often within a year of symptom onset.
“Because CJD is so rare, and the rapidly-progressive nature that struck our patient is an even more rare manifestation, I approached Dr. Ali Seifi, the director of the neurology ICU, with the idea of writing up our patient’s case as a clinical case study,” he said.
However, while doing our research, he found that the literature was lacking an updated epidemiological report on CJD in the United States.
“When discussing this with Dr. Seifi, he suggested that we fill that gap in the knowledge by writing a paper, titled ‘Creutzfeldt-Jakob Disease: In-hospital demographics report of national data in the United States from 2016 and review of a rapidly-progressive case’ that combined our patient’s case with the most recent publicly available epidemiological data on CJD using the Hospital Cost and Utilization Project,” Dr. Kotkowski said.
Link to the paper: https://authors.elsevier.com/a/1bSf9155ZJr7LJ
Among their most interesting conclusions, they found that CJD does not discriminate between men and women, rich and poor, geography, or race and ethnicity. It is distributed equally among individuals of all ethnic groups and income quartiles. They also found that 91.5 percent of patients with CJD end up being discharged to extended-care facilities or home hospice following their initial hospitalizations. This lies in contrast with their patient from University Hospital whose rapidly-progressive case led him to require intubation and eventually passed away in the Neuro ICU within two months of symptom onset.
“This paper was important to me for a variety of reasons” Dr. Kotkowski said. “As an aspiring physician scientist in the field of Neurology, I felt that this case gave me the opportunity to undertake the challenge of writing up a clinical case study in collaboration with my classmates John Cabot, Davis Payne, and John Lacci as well as discuss and analyze data that is more physician-centered than basic science-centered.”
Dr. Kotkowski is currently in his eighth and final year of UT Health San Antonio’s dual-degree M.D./Ph.D. program, the South Texas Medical Scientist Training Program, having recently begun his fourth and final year of medical school. He will be applying to neurology residency programs in the coming months while wrapping up research projects left over from his Ph.D. years in the Fox Lab at the Research Imaging Institute.
Dr, Kotkowski completed his first two years of medical school in 2015, a Ph.D. in Radiological Sciences in 2019, and is set to complete his final two years of medical school in 2021.
He has served as the 2014 Presidential Ambassadorial Scholar for the Long School of Medicine and was the 2019 recipient of the Armand Guarino Award for Academic Excellence in Doctoral Studies.
Interested in connecting with Eithan? Find him on gsbsalumni.com. In Press is a section in The Pipette Gazette that highlights publications by students. To read more In Press articles, click here.
